04 October 2020: Clinical Research
The Potential Role of Lung-Protective Ventilation in Preventing Postoperative Delirium in Elderly Patients Undergoing Prone Spinal Surgery: A Preliminary Study
Jing Wang1ABCEF, Lian Zhu2ABCEF, Yanan Li1BCE, Chunping Yin1BCE, Zhiyong Hou2CEF, Qiujun Wang1ADEG*DOI: 10.12659/MSM.926526
Med Sci Monit 2020; 26:e926526
Abstract
BACKGROUND: Postoperative delirium (POD) is a frequent complication in elderly patients, usually occurring within a few days after surgery. This study investigated the effect of lung-protective ventilation (LPV) on POD in elderly patients undergoing spinal surgery and the mechanism by which LPV suppresses POD.
MATERIAL AND METHODS: Seventy-one patients aged ≥65 years were randomized to receive LPV or conventional mechanical ventilation (MV), consisting of intermittent positive pressure ventilation following induction of anesthesia. The tidal volume in patients who received MV was 8 ml/kg predicted body weight (PBW), and the ventilation frequency was 12 times/min. The tidal volume in patients who received LPV was 6 ml/kg PBW, the positive end-expiratory pressure was 5 cmH₂O, and the ventilation frequency was 15 times/min, with a lung recruitment maneuver performed every 30 min. Blood samples were collected immediately before anesthesia induction (T₀), 10 min (T₁) and 60 min (T₂) after turning over, immediately after the operation (T₃), and 15 min after extubation (T₄) for blood gas analysis. Simultaneous cerebral oxygen saturation (rSO₂) and cerebral desaturation were recorded. Preoperative and postoperative serum concentrations of interleukin (IL)-6, IL-10 and glial fibrillary acidic protein (GFAP) were measured by ELISA. POD was assessed by nursing delirium screening score.
RESULTS: Compared with the MV group, pH was lower and PaCO₂ higher in the LPV group at T₂. In addition PaO₂, SaO₂, and PaO₂/FiO₂ were higher at T₁, and T₄, and rSO₂ was higher at T₃, and T₄ in the LPV than in the MV group (P<0.05 each). Postoperative serum GFAP and IL-6 were lower and IL-10 higher in the LPV group. The incidences of cerebral desaturation and POD were significantly lower in the LPV group (P<0.05).
CONCLUSIONS: LPV may reduce POD in elderly patients undergoing spinal surgery by inhibiting inflammation and improving cerebral oxygen metabolism.
Keywords: Cerebral Cortex, Delirium, Prone Position, Ventilation, Double-Blind Method, Emergence Delirium, Neurosurgical Procedures, Positive-Pressure Respiration, Prospective Studies
Background
Postoperative delirium (POD) is an acute and fluctuating dysfunction of consciousness caused by surgically-associated and individual patient factors. It is a common postoperative complication in the elderly, usually occurring within a few days after surgery [1]. POD is characterized by disorientation, reduce attention, and changes in cognitive function. Delirium can increase postoperative complications, prolong hospital stay, and increase financial costs. Measures to deal with delirium include prevention, monitoring, and early treatment, with prevention being better than earliest possible treatment [2,3].
The incidence of POD increases with increasing number of operations, especially in elderly patients after spinal surgery [4]. Spinal surgery is complex, delicate, and time-consuming, resulting in an incidence of POD that can be as high as 40.5% [5]. Patients undergoing spinal surgery are usually placed in a prone position, as the operating field is clear and convenient for surgery. However, this position is non-physiological, reducing cerebral oxygen saturation (rSO2). Decreased rSO2 is more likely to occur when patients are in the prone than in the supine position or when they change from the supine to the prone position [6].
Intraoperative cerebral blood flow and inadequate oxygen supply are the main risk factors for POD and cognitive dysfunction [6]. Spinal surgery in the prone position increases the risk of changes in cerebral blood perfusion, which may affect the oxygen supply to the brain [7]. The prone position also increases intra-abdominal pressure because of direct compression of the inferior vena cava and increased intrathoracic pressure. Left ventricular compliance and filling are also reduced, leading to hypotension and decreased cerebral perfusion. Reduced blood supply to the brain reduces its oxygen supply [8]. Imbalances between oxygen supply and consumption in the brain can induce brain cell hypoxia and metabolic dysfunction in brain tissue. This, in turn, can reduce the number of neurons in the brain and induce imbalances in central neurotransmitters, such as acetylcholine and dopamine, and leading to delirium [9,10].
Inflammation is also a major risk factor for POD [10–12]. Mechanical ventilation can cause ventilator-associated lung injury, which can promote the release of inflammatory factors in the lungs and throughout the body [13–15]. Because respiratory function and lung compliance are generally reduced in elderly patients, mechanical ventilation under general anesthesia is more likely to cause lung injury such as barotraumas and induce peripheral inflammatory responses. Peripheral inflammatory factors can interact with endothelial cells at the blood-brain barrier (BBB) and induce the release of other inflammatory molecules into the brain. Peripheral inflammatory factors can also activate mast cells to release pro-inflammatory factors and neurotoxic substances, which can cause the destruction of the BBB. When the BBB is destroyed, these mediators can enter the brain and activate glial cells and neurons to release various neuroinflammatory mediators. In addition, activation of microglia and astrocytes in the brain can induce their release of inflammatory mediators, which can cross the defective BBB into the peripheral system. These mediators can recruit and activate inflammatory cells near the site of brain inflammation site, exacerbating the inflammation and neurodegeneration of the brain. This, in turn can cause ischemia, hypoxia, and even edema of brain tissue, eventually resulting in neuronal injury and neurodegeneration [16–18].
Lung-protective ventilation (LPV) includes low tidal volume, a certain level of positive end-expiratory pressure (PEEP), and hypercapnia, with or without a lung recruitment maneuver [19]. LPV is mainly used in patients with acute respiratory distress syndrome (ARDS) and is increasingly used in anesthetized patients undergoing surgery. LPV can benefit patients without lung injury who require mechanical ventilation during surgery, significantly reducing the incidence of postoperative pulmonary complications [20]. Moreover, LPV during general anesthesia can improve pulmonary compliance, effectively avoid barotrauma, and ensure oxygenation [21]. The present study therefore evaluated the effect of LPV on POD in elderly patients undergoing spinal surgery in the prone position and assessed the relationships among LPV, neuroinflammation, rSO2, and POD. These results may provide clinical evidence of methods to prevent POD.
Material and Methods
PARTICIPANTS:
Using a random numbers table method, patients were randomly assigned by 2 individuals not involved in this study to undergo conventional mechanical ventilation (MV) or LPV during surgery. The anesthesiologists were not involved in the study, and the data collectors and medical staff members responsible for the preoperative and postoperative management of the patient were unaware of the intraoperative method of mechanical ventilation used for each patient. All patients underwent posterior lumbar decompression and interbody fusion with internal fixation under general anesthesia from March to September 2019 in the Third Hospital of Hebei Medical University. Patients were included if they were aged ≥65 years; had a body mass index (BMI) <28 kg/m2, an American Society of Anesthesiologists (ASA) physical status ≤III; and a score ≥23 points on the mini-mental state examination (MMSE) performed 1 day before surgery. Patients were required to have had no history of anemia, hypoalbuminemia, central nervous system disorders, mental illness, hypoxemia, chronic lung disease, asthma, or treatment with antidepressant or sedative drugs. Patients were excluded if they had baseline rSO2 <60% before anesthesia induction; their surgical plan was changed; they refused blood donations; the operation time was >4 h, or intraoperative blood loss was > 800 ml.
ANESTHESIA AND SURGICAL MANAGEMENT:
All patients were anesthetized by experienced anesthesiologists and all operations were performed by experienced spinal surgeons. After entering the operating room, blood pressure, electrocardiogram, digital pulse oxygen saturation, PETCO2, and rSO2 were monitored. Cerebral oxygen electrodes were placed on the forehead 4 cm from the eyebrow arch to avoid the frontal sinus. Measurements of rSO2 were concealed from the anesthetist so that anesthetic management was not influenced by rSO2. Intravenous anesthesia was rapidly introduced, oral visual tracheal intubation was performed for complete muscle relaxation, and intermittent positive pressure was applied for mechanical ventilation. Body temperature was maintained by intraoperative blood transfusion and infusion thermostats. Depth of anesthesia was monitored to maintain bispectral index (BIS) at 45 to 60, and doses of anesthetic drugs and fluids were adjusted based on changes in BIS and hemodynamics. Blood pressure fluctuation did not exceed 20% of its baseline amplitude. Atropine was administered only to reverse bradycardia. After extubation, all patients were transferred to the surgical intensive care unit and received inhaled oxygen at a flow of 2 L/min through a nasal catheter.
INTERVENTION METHODS:
The tidal volume of patients in the control (MV) group was set at 8 ml/kg predicted body weight (PBW), and the initial ventilation frequency was 12 times/min. In the LPV group, tidal volume was set at 6 ml/kg PBW, low-level PEEP at 5 cmH2O or 0.490 kPa, and the initial ventilation frequency at 15 times/min, with a lung recruitment maneuver performed every 30 min. Other parameters of the ventilator were the same in the 2 groups, including I: E of 1: 2, oxygen concentration of 100%, and oxygen flow of 2 L/min. PETCO2 was maintained at 35–45 mmHg (4.655–5.985 kPa) by adjusting the ventilation frequency. For lung recruitment during surgery, the peak inspiratory pressure was initially set at 45 cmH2O, tidal volume set at 8 ml/kg PBW, ventilation frequency at 6–8 times/min, I: E at 1: 2, and PEEP at 5 cmH2O [23]. The tidal volume was gradually increased by 4 ml/kg PBW until the average airway pressure was 30–35 cmH2O, and 3 consecutive breaths were taken. After the end of the operation, PEEP was maintained at 5 cmH2O, and the remaining parameters were set identical to those before lung recruitment.
BLOOD SAMPLES:
Venous blood samples were drawn into sterile EDTA-containing test tubes before the induction of anesthesia and 3 days after surgery. Four ml aliquots were allowed to coagulate at room temperature for 30 min and centrifuged at 1,000×
DATE COLLECTION AND SERUM INDEX DETECTION:
Blood samples from the radial artery were collected immediately before induction of anesthesia (T0), 10 min (T1) and 60 min (T2) after turning over, immediately after the operation (T3), and 15 min after extubation (T4). Blood gasses were analyzed; pH, PaO2, PaCO2, and SaO2 were recorded; and PaO2/SaO2 was calculated. Simultaneously, rSO2 and the incidence of cerebral desaturation during surgery were recorded. Serum concentrations of interleukin (IL)-6, IL-10, and glial fibrillary acidic protein (GFAP) were determined by commercial IL-6 (ABclonal, Woburn, MA, USA), IL-10 (ABclonal) and GFAP (CUSABIO, Houston, TX, USA) ELISA kits, respectively.
CALCULATION OF PBW:
PBW was calculated as 50 kg+0.91 kg×(height [cm]−152.4) for men and as 45.5 kg+0.91 kg×(height [cm]−152.4) for women [24].
:
The rSO2 values of each cerebral oxygen electrode were recorded within 2 minutes prior to anesthesia induction and averaged. The lower of the 2 averages was defined as the baseline rSO2 value of that patient [25]. Cerebral desaturation was defined as a reduction in rSO2 value >20% from baseline value or intraoperative rSO2 value <40% lasting for more than 1 min [26].
EVALUATION OF DELIRIUM:
POD was determined by a bedside nurse trained in neurology department using the nursing delirium screening score (Nu-DESC), performed 1–3 days postoperatively. Five parameters were captured: disorientation, inappropriate behavior, inappropriate communication, illusions/hallucinations, and psychomotor retardation, with each graded as 0–2 points. Delirium was defined as a score of ≥2 points on one of the 3 days [27].
CALCULATION OF SAMPLE SIZE: To compare the effects of LPV and conventional MV on POD in elderly patients undergoing spinal surgery, the standard deviations in the 2 groups were assumed to be equal, with a between-group difference in cognitive function defined at 75% of the standard deviation. If α=0.05 and β=0.10, then δ/σ=0.75, the formula for comparing the mean of 2 sample sizes, indicated that 31 patients were needed for each group [22]. Assuming a dropout rate of 20%, at least 74 patients should be included in both groups to ensure that 62 patients completed the study.
All data were analyzed using SPSS version 21.0 software for Windows (SPSS Inc, Chicago, IL, USA). Normally distributed data were expressed as mean±standard deviation and compared by independent-samples
Results
Of the 80 patients screened for this study, 9 did not agree to take part and 7 were excluded, including 3 with baseline rSO2 <60% before anesthesia induction; 3 because operation plans changed; and 1 who refused to supply a blood sample after the operation. Thus, this study included 64 patients, 32 in each group (Figure 1, flow diagram). Demographic and clinical characteristics did not differ significantly in the 2 groups (
Blood gas analysis, showed no significant between-group differences at T0. In contrast, pH was significantly lower (
Prior to surgery, there were no significant between-group differences in IL-6, IL-10, and GFAP concentrations. Three days after surgery, however, serum concentrations of GFAP (
Comparisons of rSO2 values in the MV group showed that, when compared with T0 on the same side, rSO2 values were significantly lower on the right side at T2 (
Comparisons of rSO2 values in the LPV group showed that rSO2 values at T4 were significantly higher on the left side than at T0 (
Discussion
This study found that the incidence of POD was significantly lower in patients who received LPV than in those who received conventional MV, suggesting that LPV, consisting of low tidal volume+5 cmH2O PEEP combined with lung recruitment, may reduce the incidence of POD in elderly patients after spinal surgery in the prone position. This strategy may lower POD by inhibiting systemic inflammation caused by lung injury and improving cerebral oxygen metabolism.
Low tidal volume and proper PEEP has significant benefits on mortality in ARDS patients [28], with patients who underwent various surgical procedures benefitting from LPV [29–31]. A ventilation mode consisting of low tidal volume (6 ml/kg) combined with low PEEP (5 cmH2O) during general anesthesia was found to effectively avoid lung injury, ensure patient oxygenation, and improve lung compliance [21]. Lung recruitment can also improve oxygenation and pulmonary compliance [32]. This preliminary study investigating the relationship between LPV and POD suggests the need for further large-scale clinical trials.
Cerebral oxygen monitoring uses near-infrared spectroscopy (NIRS) to non-invasively measure the oxygenation state of the frontal lobe of the brain, enabling evaluation of the balance between cerebral oxygen supply and consumption, as well as changes in cerebral blood flow [6,33,34]. Cerebral desaturation has been associated with postoperative cognitive dysfunction following general surgery [35,36]. Dynamic monitoring of intraoperative changes in rSO2 values, focusing on fluctuations at baseline, is of greater clinical significance than simply recording absolute rSO2 values [34]. The present study therefore measured rSO2 values at different time points and associated changes, confirming the relationships among LPV, cerebral desaturation in the prone position, and POD.
Blood acidity and PaCO2 affect the affinity of hemoglobin to oxygen, known as the Bohr effect. A reduction in pH or an increase in PaCO2 reduces the affinity of hemoglobin to oxygen, increasing the oxygen supply to tissues. At the same time, increased PaCO2 can relax cerebral blood vessels and increase cerebral blood flow [37], delivering more oxygen to brain tissues. This study found that, under conditions of ensured oxygenation, the PaCO2 of arterial blood in the LPV group increased and the pH decreased at T2. Although rSO2 did not change significantly at T2, it showed an upward trend, with significant increases at T3 and T4. These results suggest that LPV may improve cerebral oxygen metabolism through the Bohr effect.
Elevated levels of inflammatory response markers are strongly associated with delirium [38–40]. IL-6 is an acute reactive protein that can serve as a marker for surgical injury and lung injury due to ventilation [41]. High levels of IL-6 correlate with nosocomial mortality, as well as various baseline characteristics, such as poor functional status, cognitive disorders, and emergency admissions [40]. IL-10, which is mainly produced by monocytes and macrophages, can inhibit the release of pro-inflammatory factors such as tumor necrosis factor (TNF)-α, IL-6, and IL-8. Both the pro-inflammatory factor IL-6 and the anti-inflammatory factor IL-10 are closely related to POD [42].
Inflammation can increase metabolic load in the brain. Studies of premature infants have shown that exposure to inflammation in the womb leads to increased brain oxygen consumption, increasing their risk of severe hypoxia and ischemia [42]. Perinatal inflammation is associated with poor neural development, which may be due to changes in oxygen supply and consumption in the brain [43]. This study showed that LPV reduced inflammatory responses and increased rSO2 values in patients who underwent spinal surgery in the prone position, suggesting that LPV may reduce tissue oxygen consumption by reducing inflammatory responses, thereby increasing brain oxygen and reducing delirium.
Severe systemic inflammation has a strong effect on neurocognitive functions of the brain. Damage to the hippocampus appears to be directly involved in this process, while astrocytes play an important role in neuroinflammation and neuroimmune responses [44]. GFAP is a structural protein in astrocytes of the central nervous system, and its release is usually associated with stroke or acute brain injury. High levels of GFAP in the brain have been reported to correlate with the occurrence of POD [45,46]. This study found that, along with reducing the incidence of POD, LPV significantly reduced the postoperative serum concentration of GFAP compared with the conventional MV group, providing further evidence for the relationship between GFAP and delirium.
POD is thought to be caused by neurotransmitter imbalance and inflammation [47–49]. Brain tissue ischemia and hypoxia can alter central neurotransmitter content. Acetylcholine levels were shown to be reduced and dopamine levels elevated in plasma and cerebrospinal fluid of patients with delirium [50–52]. Release of acetylcholine inhibits the release of TNF-α, IL-6, and IL-8, suggesting that cholinergic anti-inflammatory effects may protect the brain from inflammatory responses. Therefore, decreased cholinergic activity can lead to neuroinflammatory responses and further cognitive impairment. Elevated dopamine can induce changes in the neurological behavior of patients with delirium by directly stimulating the central nervous system and other pathways [48]. Inflammatory mediators, which are inversely associated with the number of synapses in mouse brain, can significantly activate microglia, which are closely related to neurodegeneration [53]. During systemic inflammation, white blood cells adhere to endothelial cells, leading to the release of free radicals and enzymes, increasing BBB permeability. This allows the central nervous system to respond to surrounding immune signals, resulting in the production of cytokines and other inflammatory mediators in the brain [48,54]. This process can aggravate the inflammation of the central nervous system, resulting in cognitive function and behavioral disorders.
Because older patients with preexisting cognitive impairment are at greatest risk of delirium [47], the MMSE test was administered before surgery to eliminate patients with dementia. Moreover, lung compliance in general anesthesia is affected by many factors, resulting in the exclusion of patients with obvious thoracic and pulmonary diseases and those taking drugs that could affect lung function. Because obesity can affect ventilation mechanics in the prone position, patients with BMI >28 kg/m2 were excluded. In addition, low preoperative rSO2 (<60%) has been associated with delirium [25]; therefore, patients with baseline rSO2 value <60% before anesthesia induction were excluded from this study.
This study had several limitations. Because of the strict exclusion criteria, the number of patients enrolled was small. Changes in cognitive function may also result from preoperative medication, pain, and postoperative use of analgesics or other medications. This pilot study utilized univariate analysis to study the relationship between LPV and POD. A larger clinical trial is needed, enabling multivariate analysis that can control for potential confounders. Inflammatory indicators in bronchoalveolar lavage fluid can better reflect the degree of lung injury, as can serum CC16 [55], suggesting that future clinical studies should assess additional numbers of lung injury indicators. It is also necessary to monitor indicators of respiratory mechanics during ventilation. The patient follow-up time of this study was short, suggesting that prolonged observation may help better guide the management of delirium in these patients. The ability to assess cognitive status in elderly patients is also limited. The Nu-DESC test, which has high sensitivity but low specificity, is administered by a nurse at the bedside as part of their daily practice of clinical management [27]. Although serum concentrations of inflammatory factors were measured, serum may not adequately reflect the concentrations of these factors in cerebrospinal fluid. Peripheral inflammation may alter the inflammation of the central nervous system by means other than increasing BBB permeability. This study did not measure changes in central neurotransmitter content, suggesting the need for further clinical studies to confirm the relationships of LPV, delirium after surgery in the prone position, and neurotransmitter imbalances.
Conclusions
LPV is potentially beneficial for elderly patients undergoing spinal surgery in the prone position, via a mechanism that involves reduced inflammatory responses and improved cerebral oxygen metabolism. The beneficial role of LPV in improving long-term treatment outcomes is unclear, indicating a need for further research to elucidate the mechanisms by which LPV inhibits the development of POD.
Figures
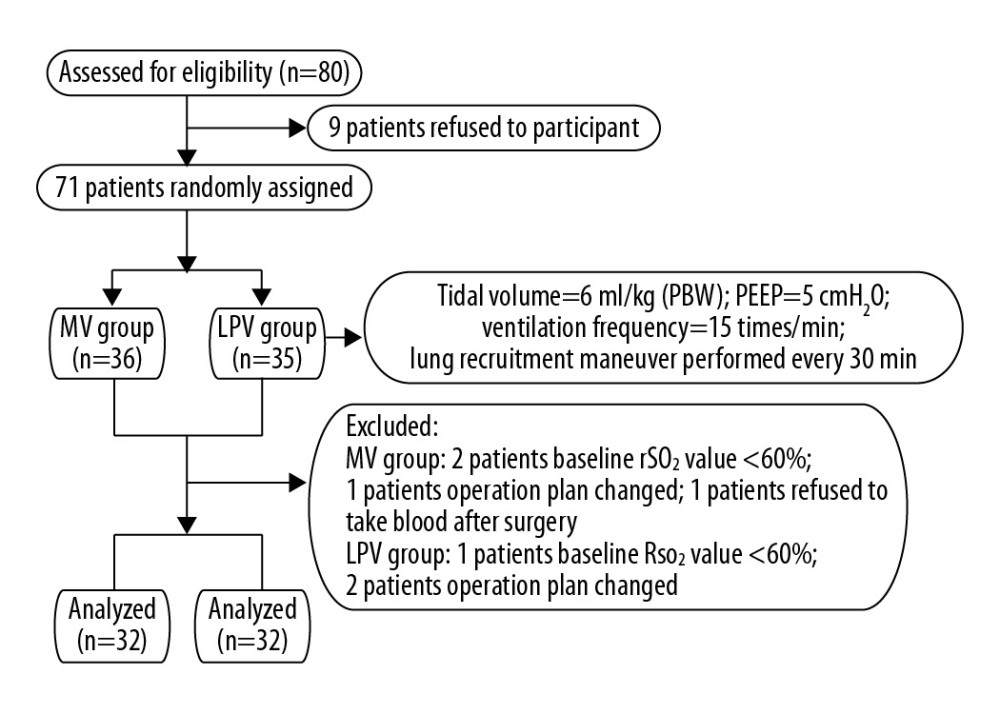 Figure 1. Patient flow diagram of this study. Studies have found that preoperative rSO2 value less than 60% is closely related to the occurrence of postoperative mental state dysfunction in elderly patients, therefore, patients with baseline rSO2 value <60% before anesthesia induction were removed from the trial. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation.
Figure 1. Patient flow diagram of this study. Studies have found that preoperative rSO2 value less than 60% is closely related to the occurrence of postoperative mental state dysfunction in elderly patients, therefore, patients with baseline rSO2 value <60% before anesthesia induction were removed from the trial. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation. 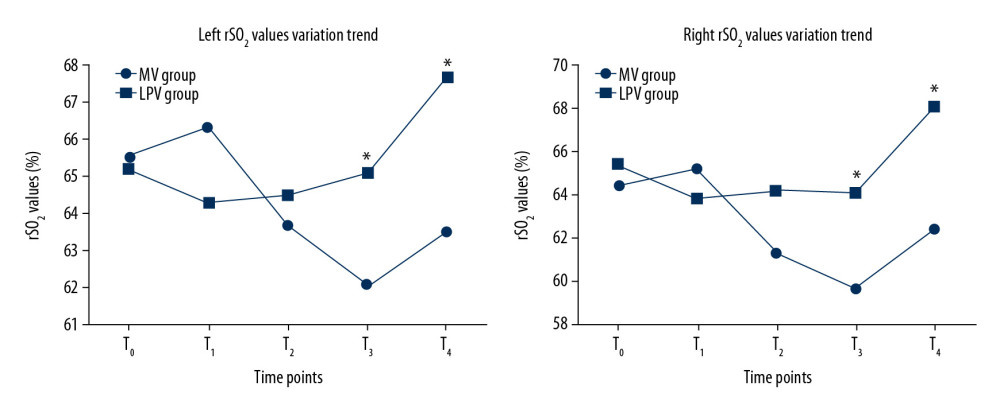 Figure 2. Changes over time in rSO2 values on the left and right sides in patients who received LPV or conventional MV. Compared with MV group, * P<0.05. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation; T0 – immediately before anesthesia induction; T1 – 10 min after turning over; T2 – 60 min after turning over; T3 – immediately after operation; T4 – 15 min after extubation.
Figure 2. Changes over time in rSO2 values on the left and right sides in patients who received LPV or conventional MV. Compared with MV group, * P<0.05. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation; T0 – immediately before anesthesia induction; T1 – 10 min after turning over; T2 – 60 min after turning over; T3 – immediately after operation; T4 – 15 min after extubation. Tables
Table 1. Demographic and clinical characteristics of patients who received LPV or conventional MV and rates of cerebral desaturation and postoperative delirium (POD).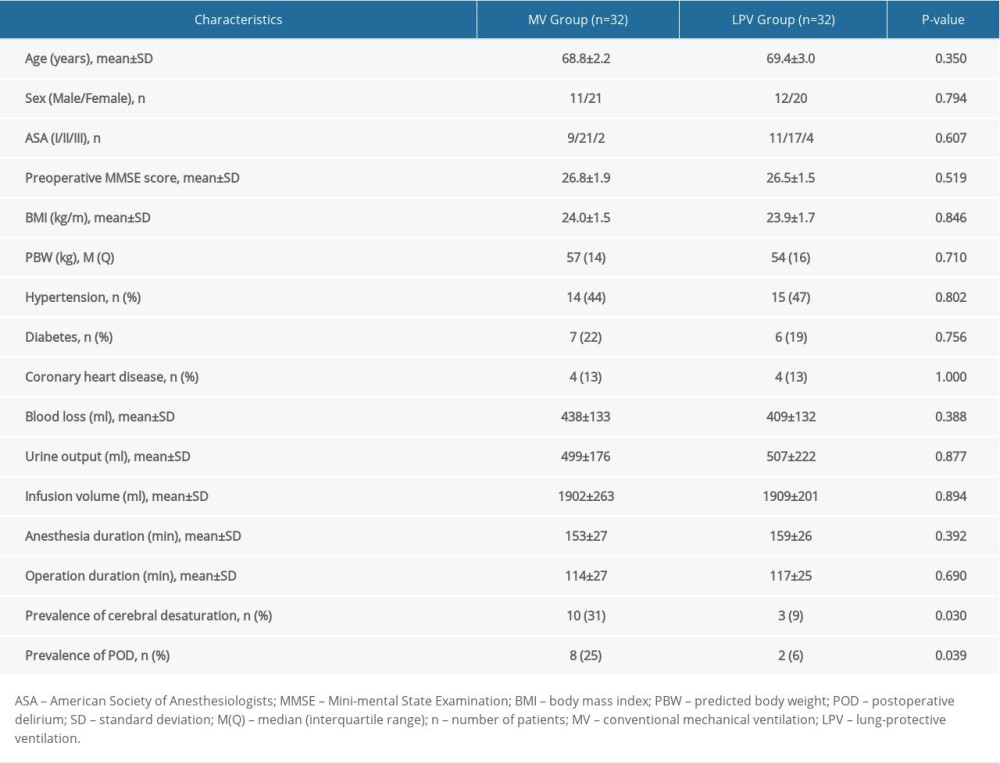 Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each).
Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each).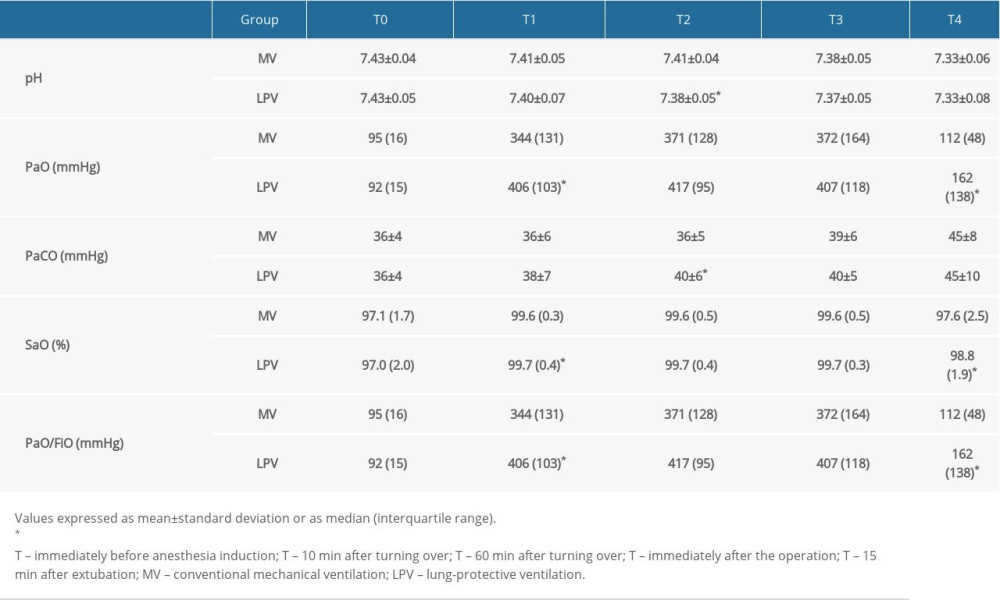 Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each).
Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each).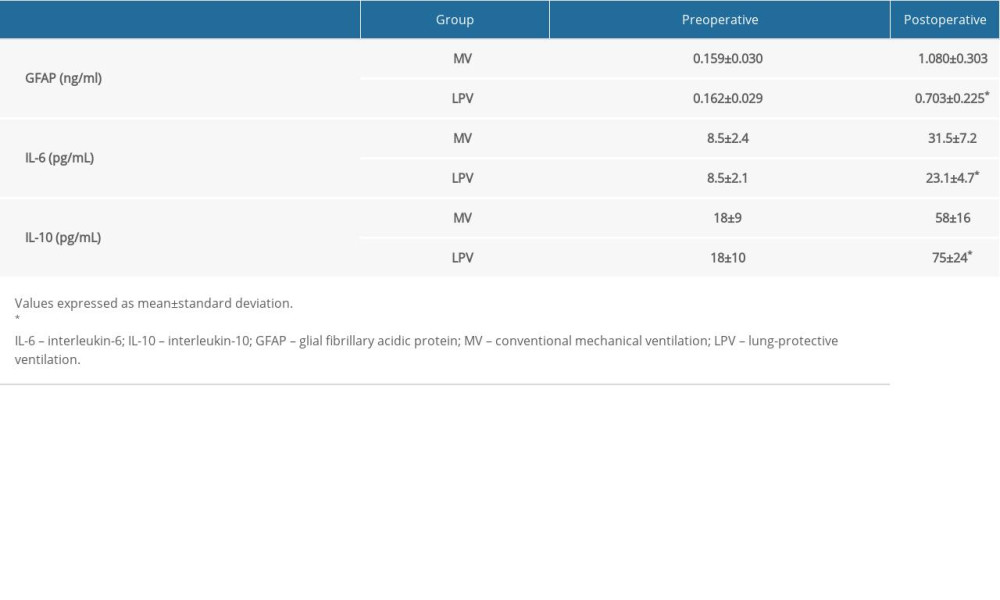
References
1. Javedan H, Tulebaev S, Management of common postoperative complications: Delirium: Clin Geriatr Med, 2014; 30(2); 271-78
2. Strøm C, Rasmussen LS, Challenges in anaesthesia for elderly: Singapore Dent J, 2014; 35C; 23-29
3. Silverstein JH, Timberger M, Reich DL, Uysal S, Central nervous system dysfunction after noncardiac surgery and anesthesia in the elderly: Anesthesiology, 2007; 106(3); 622-28
4. Brown CH, Jones EL, Lin C, Shaping anesthetic techniques to reduce post-operative delirium (SHARP) study: A protocol for a prospective pragmatic randomized controlled trial to evaluate spinal anesthesia with targeted sedation compared with general anesthesia in older adults undergoing lumbar spine fusion surgery: BMC Anesthesiol, 2019; 19(1); 192
5. Brown CH, LaFlam A, Max L, Delirium after spine surgery in older adults: Incidence, risk factors, and outcomes: J Am Geriatr Soc, 2016; 64(10); 2101-8
6. Deiner S, Chu I, Mahanian M, Prone position is associated with mild cerebral oxygen desaturation in elderly surgical patients: PLoS One, 2014; 9(9); e106387
7. Closhen D, Engelhard K, Dette F, Changes in cerebral oxygen saturation following prone positioning for orthopaedic surgery under general anaesthesia: A prospective observational study: Eur J Anaesthesiol, 2015; 32(6); 381-86
8. Murniece S, Soehle M, Vanags I, Mamaja B, Near infrared spectroscopy based clinical algorithm applicability during spinal neurosurgery and postoperative cognitive disturbances: Medicina (Kaunas), 2019; 55(5); 179
9. Mulkey MA, Hardin SR, Olson DM, Munro CL, Pathophysiology review: Seven neurotransmitters associated with delirium: Clin Nurse Spec, 2018; 32(4); 195-211
10. Maldonado JR, Neuropathogenesis of delirium: Review of current etiologic theories and common pathways: Am J Geriatr Psychiatry, 2013; 21(12); 1190-222
11. Wolters AE, Peelen LM, Veldhuijzen DS, Long-term self-reported cognitive problems after delirium in the intensive care unit and the effect of systemic inflammation: J Am Geriatr Soc, 2017; 65(4); 786-91
12. Hshieh TT, Vasunilashorn SM, D’Aquila MLRISE Study Group, The Role of Inflammation after Surgery for Elders (RISE) study: Study design, procedures, and cohort profile: Alzheimers Dement (Amst), 2019; 11; 752-62
13. Pinhu L, Whitehead T, Evans T, Griffiths M, Ventilator-associated lung injury: Lancet, 2003; 361(9354); 332-40
14. Boehm O, Rohner M, Ehrentraut H, Low-tidal-volume prevent ventilation induced inflammation in a mouse model of sepsis: Life Sci, 2020; 240; 117081
15. Plötz FB, Slutsky AS, van Vught AJ, Heijnen CJ, Ventilator-induced lung injury and multiple system organ failure: A critical review of facts and hypotheses: Intensive Care Med, 2004; 30(10); 1865-72
16. Kempuraj D, Thangavel R, Selvakumar GP, Brain and peripheral atypical inflammatory mediators potentiate neuroinflammation and neurodegeneration: Front Cell Neurosci, 2017; 11; 216
17. Dong R, Sun L, Lu Y, NeurimmiRs and postoperative delirium in elderly patients undergoing total hip/knee replacement: A pilot study: Front Aging Neurosci, 2017; 9; 200
18. Teeling JL, Perry VH, Systemic infection and inflammation in acute CNS injury and chronic neurodegeneration: Underlying mechanisms: Neuroscience, 2009; 158(3); 1062-73
19. Tang L, Kazan R, Taddei R, Reduced cerebral oxygen saturation during thoracic surgery predicts early postoperative cognitive dysfunction: Br J Anaesth, 2012; 108(4); 623-29
20. Hemmes SNT, Neto AS, Schultz MJ, Intraoperative ventilatory strategies to prevent postoperative pulmonary complications: A meta-analysis: Curr Opin Anaesthesiol, 2013; 26(2); 126-33
21. Sundaresan A, Chase JG, Shaw GM, Model-based optimal PEEP in mechanically ventilated ARDS patients in the intensive care unit: Biomed Eng Online, 2011; 10; 64
22. Sun ZQ, Xu YY: Medical statistics, 2010, China (Beijing), People’s Medical Publishing House
23. Hemmes SN, Severgnini P, Jaber S, Rationale and study design of PROVHILO – a worldwide multicenter randomized controlled trial on protective ventilation during general anesthesia for open abdominal surgery: Trials, 2011; 12; 111
24. Jia Y, Leung SM, Turan A, Low tidal volumes are associated with slightly improved oxygenation in patients having cardiac surgery: A cohort analysis: Anesth Analg, 2020; 130(5); 1396-406
25. Soh S, Shim JK, Song JW, Preoperative transcranial Doppler and cerebral oximetry as predictors of delirium following valvular heart surgery: A case-control study: J Clin Monit Comput, 2020; 34(4); 715-23
26. Oh CS, Sa M, Park HJ, Effects of remote ischemic preconditioning on regional cerebral oxygen saturation in patients in the beach chair position during shoulder surgery: A double-blind randomized controlled trial: J Clin Anesth, 2020; 61; 109661
27. Stukenberg S, Franck M, Spies CD, How can postoperative delirium be predicted in advance? A secondary analysis comparing three methods of early assessment in elderly patients: Minerva Anestesiol, 2016; 82(7); 751-59
28. Brower RG, Matthay MA, Morris AAcute Respiratory Distress Syndrome Network, Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome: N Engl J Med, 2000; 342(18); 1301-8
29. Spieth PM, Güldner A, Uhlig CPROtective Ventilation (PROVE) Network, Variable versus conventional lung protective mechanical ventilation during open abdominal surgery (PROVAR): A randomised controlled trial: Br J Anaesth, 2018; 120(3); 581-91
30. Park SJ, Kim BG, Oh AH, Effects of intraoperative protective lung ventilation on postoperative pulmonary complications in patients with laparoscopic surgery: Prospective, randomized and controlled trial: Surg Endosc, 2016; 30(10); 4598-606
31. Hodgson LE, Murphy PB, Hart N, Respiratory management of the obese patient undergoing surgery: J Thorac Dis, 2015; 7(5); 943-52
32. Sud S, Friedrich JO, Adhikari NK, Effect of prone positioning during mechanical ventilation on mortality among patients with acute respiratory distress syndrome: A systematic review and meta-analysis: CMAJ, 2014; 186(10); E381-90
33. Kobayashi K, Kitamura T, Kohira S, Factors associated with a low initial cerebral oxygen saturation value in patients undergoing cardiac surgery: J Artif Organs, 2017; 20(2); 110-16
34. Denault A, Deschamps A, Murkin JM, A proposed algorithm for the intraoperative use of cerebral near-infrared spectroscopy: Semin Cardiothorac Vasc Anesth, 2007; 11(4); 274-81
35. Ballard C, Jones E, Gauge N, Optimised anaesthesia to reduce post operative cognitive decline (POCD) in older patients undergoing elective surgery, a randomised controlled trial: PLoS One, 2012; 7(6); e37410
36. Casati A, Fanelli G, Pietropaoli P, Continuous monitoring of cerebral oxygen saturation in elderly patients undergoing major abdominal surgery minimizes brain exposure to potential hypoxia: Anesth Analg, 2005; 101(3); 740-47
37. Zhu DN, Wang TH: Physiology, 2013, China (Beijing), People’s Medical Publishing House
38. Girard TD, Ware LB, Bernard GR, Associations of markers of inflammation and coagulation with delirium during critical illness: Intensive Care Med, 2012; 38(12); 1965-73
39. Capri M, Yani SL, Chattat R, Pre-operative, high-IL-6 blood level is a risk factor of post-operative delirium onset in old patients: Front Endocrinol (Lausanne), 2014; 5; 173
40. Xin X, Xin F, Chen X, Hypertonic saline for prevention of delirium in geriatric patients who underwent hip surgery: J Neuroinflammation, 2017; 14(1); 221
41. Michelet P, D’Journo XB, Roch A, Protective ventilation influences systemic inflammation after esophagectomy: A randomized controlled study: Anesthesiology, 2006; 105(5); 911-19
42. Stark MJ, Hodyl NA, Belegar VKK, Andersen CC, Intrauterine inflammation, cerebral oxygen consumption and susceptibility to early brain injury in very preterm newborns: Arch Dis Child Fetal Neonatal Ed, 2016; 101(2); F137-42
43. Andersen CC, Pillow JJ, Gill AW, The cerebral critical oxygen threshold of ventilated preterm lambs and the influence of antenatal inflammation: J Appl Physiol, 2011; 111(3); 775-81
44. Bellaver B, Dos Santos JP, Leffa DT, Systemic inflammation as a driver of brain injury: The astrocyte as an emerging player: Mol Neurobiol, 2018; 55(3); 2685-95
45. Rappold T, Laflam A, Hori D, Evidence of an association between brain cellular injury and cognitive decline after non-cardiac surgery: Br J Anaesth, 2016; 116(1); 83-89
46. Fang KY, Zhu Y, Feng YP, Accuracy of serum S-100β protein and neuron specific enolase level in prediction of postoperative delirium in different age patients: Chin J Anesthesiol, 2012; 32(1); 27-30
47. Inouye SK, Delirium in older persons: N Engl J Med, 2006; 354(11); 1157-65
48. Wang Y, Shen X, Postoperative delirium in the elderly: The potential neuropathogenesis: Aging Clin Exp Res, 2018; 30(11); 1287-95
49. Page VJ, Casarin A, Ely EW, Evaluation of early administration of simvastatin in the prevention and treatment of delirium in critically ill patients undergoing mechanical ventilation (MoDUS): A randomised, double-blind, placebo-controlled trial: Lancet Respir Med, 2017; 5(9); 727-37
50. Trzepacz PT, Anticholinergic model for delirium: Semin Clin Neuropsychiatry, 1996; 1(4); 294-303
51. Golinger RC, Peet T, Tune LE, Association of elevated plasma anticholinergic activity with delirium in surgical patients: Am J Psychiatry, 1987; 144(9); 1218-20
52. Trzepacz PT, Leavitt M, Ciongoli K, An animal model for delirium: Psychosomatics, 1992; 33(4); 404-15
53. Murray C, Sanderson DJ, Barkus C, Systemic inflammation induces acute working memory deficits in the primed brain: Relevance for delirium: Neurobiol Aging, 2012; 33(3); 603-16
54. Nguyen DN, Spapen H, Su F, Elevated serum levels of S-100beta protein and neuron-specific enolase are associated with brain injury in patients with severe sepsis and septic shock: Crit Care Med, 2006; 34(7); 1967-74
55. Wutzler S, Lehnert T, Laurer H, Circulating levels of Clara cell protein 16 but not surfactant protein D identify and quantify lung damage in patients with multiple injuries: J Trauma, 2011; 71(2); E31-36
Figures
 Figure 1. Patient flow diagram of this study. Studies have found that preoperative rSO2 value less than 60% is closely related to the occurrence of postoperative mental state dysfunction in elderly patients, therefore, patients with baseline rSO2 value <60% before anesthesia induction were removed from the trial. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation.
Figure 1. Patient flow diagram of this study. Studies have found that preoperative rSO2 value less than 60% is closely related to the occurrence of postoperative mental state dysfunction in elderly patients, therefore, patients with baseline rSO2 value <60% before anesthesia induction were removed from the trial. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation. Figure 2. Changes over time in rSO2 values on the left and right sides in patients who received LPV or conventional MV. Compared with MV group, * P<0.05. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation; T0 – immediately before anesthesia induction; T1 – 10 min after turning over; T2 – 60 min after turning over; T3 – immediately after operation; T4 – 15 min after extubation.
Figure 2. Changes over time in rSO2 values on the left and right sides in patients who received LPV or conventional MV. Compared with MV group, * P<0.05. MV – conventional mechanical ventilation; LPV – lung-protective ventilation; rSO2 – cerebral oxygen saturation; T0 – immediately before anesthesia induction; T1 – 10 min after turning over; T2 – 60 min after turning over; T3 – immediately after operation; T4 – 15 min after extubation. Tables
 Table 1. Demographic and clinical characteristics of patients who received LPV or conventional MV and rates of cerebral desaturation and postoperative delirium (POD).
Table 1. Demographic and clinical characteristics of patients who received LPV or conventional MV and rates of cerebral desaturation and postoperative delirium (POD). Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each).
Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each). Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each).
Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each). Table 1. Demographic and clinical characteristics of patients who received LPV or conventional MV and rates of cerebral desaturation and postoperative delirium (POD).
Table 1. Demographic and clinical characteristics of patients who received LPV or conventional MV and rates of cerebral desaturation and postoperative delirium (POD). Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each).
Table 2. Blood gas parameters over time in patients who received LPV or conventional MV (n=32 each). Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each).
Table 3. Preoperative and postoperative concentrations of GFAP, IL-6, and IL-10 in patients who received LPV or conventional MV (n=32 each). In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








