16 September 2020: Clinical Research
Short-Term Outcomes of Laparoscopic Duodenum-Preserving Total Pancreatic Head Resection Compared with Laparoscopic Pancreaticoduodenectomy for the Management of Pancreatic-Head Benign or Low-Grade Malignant Lesions
Xuemin Chen1ADG, Weibo Chen1BEG, Yue Zhang1BC, Yong An1B, Xiaoying Zhang2ADF*DOI: 10.12659/MSM.927248
Med Sci Monit 2020; 26:e927248
Abstract
BACKGROUND: Several studies have shown that laparoscopic duodenum-preserving total pancreatic head resection (LDPPHRt) is safe, effective, and feasible for the management of pancreatic-head benign or low-grade malignant lesions. However, there are no studies comparing the short-term outcomes between LDPPHRt and laparoscopic pancreaticoduodenectomy (LPD). The present study aimed to evaluate the differences in the intraoperative data, postoperative data, short-term complications, and 90-day mortality rates between LDPPHRt and LPD in the management of pancreatic-head benign or low-grade malignant tumors.
MATERIAL AND METHODS: Between January 2016 and December 2019, 15 LDPPHRt and 39 LPD procedures were performed. The preoperative, intraoperative, and postoperative data were retrospectively analyzed and compared.
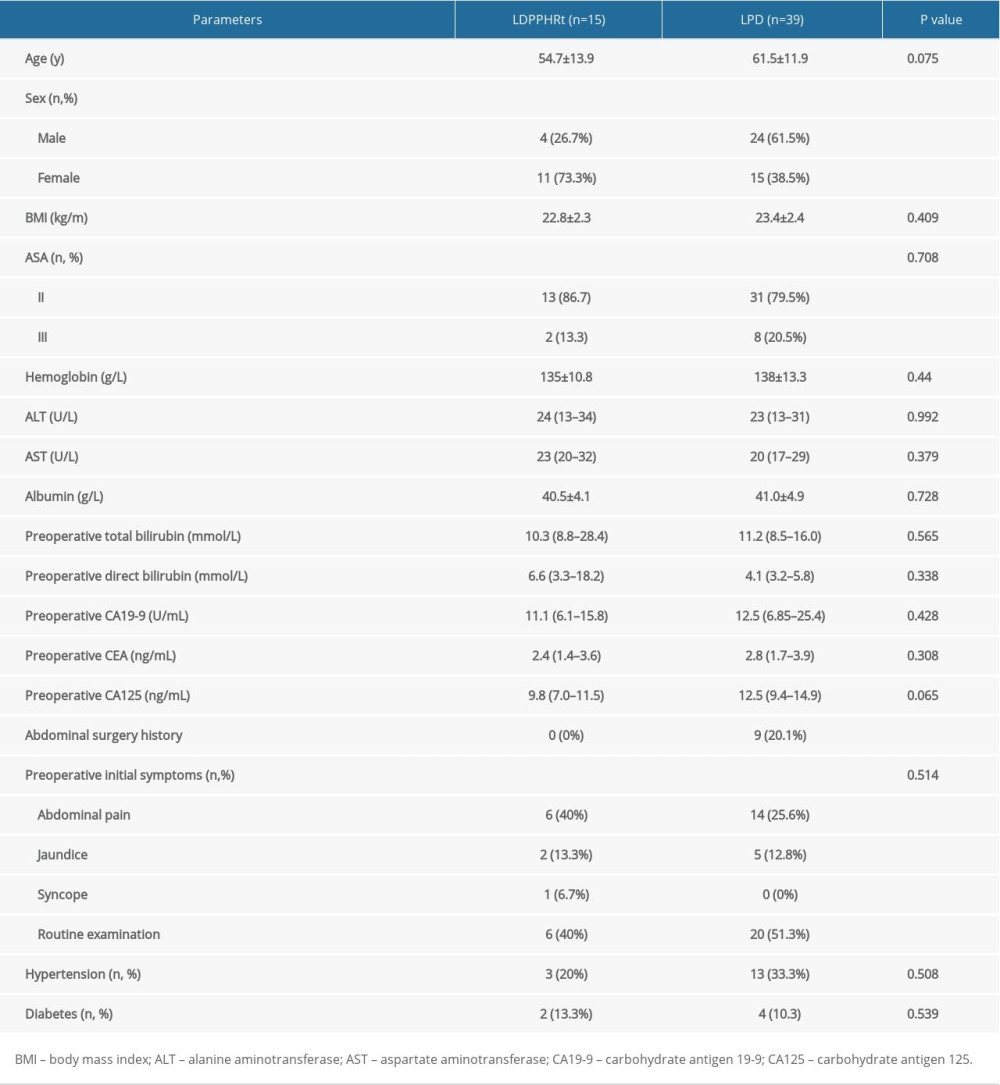
RESULTS: All of the patients received laparoscopic procedures successfully and without conversion. There were no differences in the patients’ age, body mass index, American Society of Anaesthesiologists score, preoperative examination results, preoperative initial symptoms, comorbidities, intraoperative blood loss, postoperative stay, short-term complications, 30-day readmission rates, or 90-day mortality rates. More female patients underwent LDPPHRt than LPD (73.3% vs. 38.5%; P=0.033), and no patients in the LDPPHRt group had previously undergone abdominal surgery (0% vs. 20.1%; P=0.049). The operative time was shorter in the LDPPHRt group than in the LPD group (295±42 vs. 357±87 min; P=0.011). The lesion diameter did not differ significantly between the 2 groups (2.93±1.18 vs. 2.53±1.12 cm; P=0.252). The lesion resection margins were all histopathologically negative. The distribution of pathological diagnosis was comparable in both groups. The LDPPHRt group had 4 cases of intraductal papillary mucinous neoplasm (IPMN) (26.7%), 1 case of solid pseudopapillary tumor (SPN) (6.7%), 2 cases of pancreatic neuroendocrine neoplasm (PNET) (13.3%), 2 cases of serous cystic adenoma (SCA) (13.3%), 4 cases of mucinous cystic neoplasm (MCN) (26.7%), and 2 cases of chronic pancreatitis (13.3%). The LPD group had 21 cases of IPMN (53.8%), 2 cases of SPN (5.1%), 7 cases of PNET (17.9%), 3 cases of SCA (7.7%), 2 cases of MCN (5.1%), and 4 cases of chronic pancreatitis (10.3%).
CONCLUSIONS: LDPPHRt is a time-saving procedure with short-term outcomes comparable to those of LPD for the management of benign or low-grade malignancies of the pancreatic head.
Keywords: Common Bile Duct, Laparoscopy, Total Pancreatic Head Resection, Duodenum Preservation, Duodenum, Pancreas, Pancreatic Neoplasms, Pancreaticoduodenectomy
Background
In recent years, with the rapid development of diagnostic imaging technologies, an increasing number of benign or low-grade pancreatic tumors are being diagnosed. Using pancreatic cystic lesions as an example, the serendipitous diagnosis rate from computed tomography (CT) is ~2.6%, whereas the serendipitous diagnosis rate from magnetic resonance imaging (MRI) is as high as 13.5% [1,2].
Laparoscopic pancreaticoduodenectomy (LPD) is an important surgical method for the treatment of benign or low-grade malignant tumors located in the head of the pancreas. Lee et al. showed that LPD was a safe procedure and that patients experienced less postoperative pain than with open pancreaticoduodenectomy (OPD), thus shortening hospitalization time for benign and borderline malignant periampullary disease [3]. In addition to LPD, parenchyma-sparing procedures have always garnered noticeable interest for the treatment of benign or low-grade pancreatic tumors. Surgical methods, including local resection, Beger operation, Frey operation, Izbicki operation, Berne modification, Hamburg modification, and duodenum-preserving pancreatic-head resection (DPPHR), amongst others, maximize the preservation of normal pancreatic parenchyma and maintain the integrity of the digestive tract as much as possible, with little impact on sugar metabolism and digestive function [4].
DPPHR was first introduced in 1972 for the management of inflammatory masses situated in the pancreatic head [5]. Regarding short-term and long-term outcomes, DPPHR was comparable to pancreaticoduodenectomy (PD) and even exhibited improved outcomes with regard to perioperative and postoperative outcome parameters, including intraoperative hemorrhage and duration of hospitalization [6]. Based on the extent of the pancreatic-head resection, DPPHR may be classified as total (DPPHRt) or partial (DPPHRp). In 1994, Nakao et al. described DPPHRt with segmental resection of the peripapillary duodenum [3], and in 1999, Beger et al. reported DPPHRt without segmental duodenum resection [4].
Recent advancements in DPPHRt have been attributed to the improvement of minimally invasive technologies. In 2019, Cao et al. reported 12 cases of laparoscopic DPPHRt (LDPPHRt) for the management of benign or low-grade malignant tumors of the pancreatic head, with favorable outcomes [5]. LDPPHRt combines the advantages of DPPHRt with a minimally invasive procedure, but requires meticulous and precise intraoperative techniques to preserve the duodenal blood supply and the common bile duct (CBD).
To the best of our knowledge, there have been no studies to date comparing LDPPHRt and LPD for the management of pancreatic-head benign or low-grade malignant tumors. This study aimed to evaluate the differences in the short-term outcomes between patients who underwent LDPPHRt and LPD.
Material and Methods
PATIENTS:
Between January 2016 and December 2019, 15 LDPPHRt procedures for patients with benign or low-grade malignant pancreatic-head lesions were performed at the Department of Hepatopancreatobiliary Surgery at the Third Affiliated Hospital of Soochow University.
In addition, 39 patients who received LPD were enrolled in this retrospective study. The selection criteria for LDPPHRt or LPD were as follows: i) Patients were diagnosed with pancreatic-head benign or low-grade lesions, including intraductal papillary mucinous neoplasm (IPMN), serous cystic adenoma (SCA), mucinous cystic neoplasm (MCN), pancreatic neuroendocrine neoplasm (PNET), or solid pseudopapillary tumor (SPN). All of the patients were evaluated by preoperative CT scan and/or magnetic resonance imaging (MRI) and serum tumor marker tests to rule out pancreatic malignancies. ii) Resectability of the tumors was confirmed based on preoperative radiology. Patients who had an American Society of Anaesthesiologists (ASA) score >3 points and those who could not tolerate pneumoperitoneum pressure were excluded from this study. For LDPPHRt, the lesions must not be located too close to the intrapancreatic CBD or the inferior pancreatic arcades. Patients with a history of chronic pancreatitis, which may be correlated with severe pancreatic fibrosis and peripancreatic adhesion, were not included in the LDPPHRt group. The present study was approved by the Ethics Committee of the Third Affiliated Hospital of Soochow University, and was performed in accordance with the relevant guidelines and regulations. Informed consent was obtained from all participants.
DATA COLLECTION:
The demographic data, preoperative examination results, pathological diagnosis, and short-term outcomes, such as operative time, estimated blood loss, postoperative hospitalization time, and complications [including postoperative pancreatic fistula (POPF), bile leakage, delayed gastric emptying (DGE), abdominal infection, and hemorrhage] were recorded and analyzed. POPF was classified based on the updated definition and classification by the International Study Group of Pancreatic Fistula in 2016 [6]. DGE was diagnosed according to the criteria defined by the International Study Group of Pancreatic Surgery published in 2007 [7].
LDPPHRT:
The operation was performed under general anesthesia with prophylactic intravenous antibiotics. The patient was placed in a supine position with the legs separated, upper body leaning forward 30° and a left/right tilting of 15° according to the intraoperative needs. The operating surgeon stood on the right side and the assistant surgeon on the left. The camera surgeon stood between the legs of the patient. The pneumoperitoneum was established with carbon dioxide at a pressure of 12 mmHg. The 5 trocars were placed in a U shape with a 12-mm trocar under the umbilical cord for laparoscopy.
A systematic and meticulous examination of the peritoneal cavity was performed to rule out possible malignancies and metastases. The liver was hung to the anterior abdominal wall to expose the gastrocolic omentum, which was opened to visualize the pancreatic head and body. The location, size, and mobility of the lesion were noted. The inferior and superior edges of the pancreatic neck were dissected to expose the superior mesenteric vein (SMV) and the common hepatic artery (CHA), respectively. The CHA was aligned to remove the group 8a lymph nodes, and the gastroduodenal artery (GDA) was identified. A tunnel was established behind the pancreatic neck by blunt separation. The pancreatic neck was transected along the right side of the portal vein (PV) using a harmonic scalpel, and the main pancreatic duct (MPD) was located. The pancreatic head was pulled to the right to separate the connection to the right and dorsal edges of the SMV and to expose the right-side tract of the superior mesenteric artery. After total detachment from the SMV, the pancreatic-head capsule was opened along the second and third segments of the duodenum. The dissection was made close to the pancreatic head to preserve the anterior and the posterior inferior pancreaticoduodenal arteries while dissecting the inferior portion of the pancreatic head and the uncinate process. The management of the superior pancreatic head started with careful tracing down the GDA to the bifurcation where the anterior and the posterior superior pancreaticoduodenal arteries (ASPDA and PSPDA) meet. The ASPDA was resected if the mobilization of the pancreatic head was difficult, but the PSPDA was always preserved. Special attention was paid to the PSPDA ascending from the CHA. For the dissection of the intrapancreatic CBD, the pancreatic head was rotated to the right by 90°. After the rotation, the distal portion of the retro-duodenal CBD could be visualized in the triangle formed by the left edge of the GDA, the right edge of the PV, and the superior edge of the pancreas, termed as the inferior CBD triangle (Figure 1A, 1B). The pancreatic parenchyma was cut through to the left side of the CBD wall from top to bottom using an electric hook or scissors. The anterior CBD wall was dissected to expose the MPD, and then the pancreatic head was pulled down to resect the parenchyma between the duodenum and the right CBD wall. Because it is difficult to remove all the pancreatic parenchyma from the posterior CBD wall, dissections were performed carefully to protect the PSPDA. Dissection of the CBD was made away from the CBD wall to preserve the nourishing blood vessels. Thereafter, the MPD was cut and the pancreatic head and uncinate process were completely removed (Figure 2A, 2B). The MPD was sutured with 4-0 Vicryl (Johnson & Johnson, New Brunswick, NJ, USA) and hemostasis was carefully conducted. After confirming suitable blood supply of the CBD, a Roux-en-Y end-to-side duct-to-mucosa pancreaticojejunostomy was performed. A side-to-side jejunojejunostomy was made using an ECHELON FLEX60 Powered Plus Articulating Endoscopic Linear Cutter (Johnson & Johnson, New Brunswick, NJ, USA), and the wound in the jejunum was closed using a 4-0 Covidien V-loc (Covidien, Princeton, NJ, USA). Two drainage catheters were placed at the upper and lower portions of the pancreaticojejunostomy, and fixed at the right middle axillary line.
LPD: LPD was performed as reported in our previously published study [8]. In general, resection was performed using the artery-first approach following the classical Whipple’s resection rather than the pylorus-preserving technique. End-to-side duct-to-mucosa pancreaticojejunostomy was performed as in LDPPHRt. The bilioenteric anastomosis was performed using a single-layer continuous suture with 4-0 STRATAFIX (Johnson & Johnson, New Brunswick, NJ, USA). The gastrointestinal anastomosis was performed with an ECHELON FLEX60 Powered Plus Articulating Endoscopic Linear Cutter (Johnson & Johnson, New Brunswick, NJ, USA).
STATISTICAL ANALYSIS:
Statistical analysis was performed using SPSS version 20.0 (IBM). Continuous variables with a normal distribution were expressed as the mean±standard deviation, and an independent samples
Results
PATIENT CHARACTERISTICS:
In total, 15 patients who received LDPPHRt and 39 patients who received LPD were enrolled in the present study. The mean age was 54.7±13.9 years in the LDPPHRt group and 61.5±11.9 years in the LPD group (P=0.075). The proportion of female patients was 73.3% in the LDPPHRt group and 38.5% in the LPD group (P=0.033). The BMI was 22.8±2.3 kg/m2 in the LDPPHRt group and 23.4±2.4 kg/m in the LPD group (P=0.409). A total of 13 (86.7%) and 31 patients (79.5%) were classified as ASA II in the LDPPHRt and LPD groups, respectively. There were no significant differences between the 2 groups in terms of preoperative hemoglobin, alanine aminotransferase, aspartate aminotransferase, albumin, total bilirubin, direct bilirubin, carbohydrate antigen 19-9, carcinoembryonic antigen, or CA125 levels. The abdominal surgery history was different in the 2 groups: 20.1% of the patients in the LPD group had previously received abdominal surgery, while no patients had undergone abdominal surgery in the LDPPHRt group (P=0.049). Abdominal pain and routine examination findings were the predominant initial presentations. The incidence of comorbidities such as hypertension and diabetes did not differ significantly between the 2 groups. The patient characteristics are presented in Table 1.
SHORT-TERM OUTCOMES:
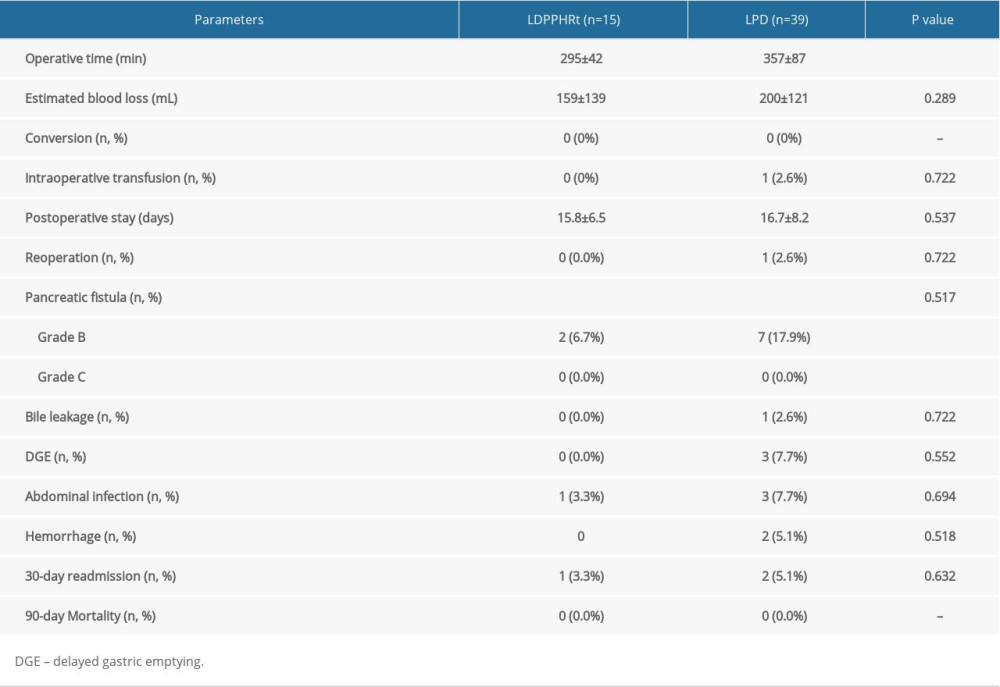
The operative time was shorter in the LDPPHRt group than in the LPD group (295±42 vs. 357±87 min; P=0.011). No significant differences were observed in estimated blood loss or intraoperative transfusion. There was no conversion in either of the groups, and the postoperative stay was comparable between the 2 groups (15.8±6.5 vs. 16.7±8.2 days; P=0.537). One patient in the LPD group underwent a reoperation due to a postoperative hemorrhage. The major complications observed were POPF, bile leakage, DGE, abdominal infection, and hemorrhage, and there were no significant differences between the 2 groups in terms of the number of complications. In the LDPPHRt group, 2 patients (6.7%) developed grade-B pancreatic fistulas and 1 patient (3.3%) developed an abdominal infection. No patients developed bile leakage, DGE, or hemorrhage. In the LPD group, there were 7 cases (17.9%) of grade-B pancreatic fistula, 1 case (2.6%) of bile leakage, 3 cases (7.7%) of DGE, 3 cases (7.7%) of abdominal infection, and 2 cases (5.1%) of hemorrhage. In the LDPPHRt group, 1 patient (3.3%) was readmitted to the hospital within 30 days due to fever. In the LPD group, 2 patients (5.1%) were readmitted due to delayed DGE and malnutrition. No patients died of any cause in the 90-day follow-up period in either group (Table 2).
PATHOLOGICAL DIAGNOSIS:
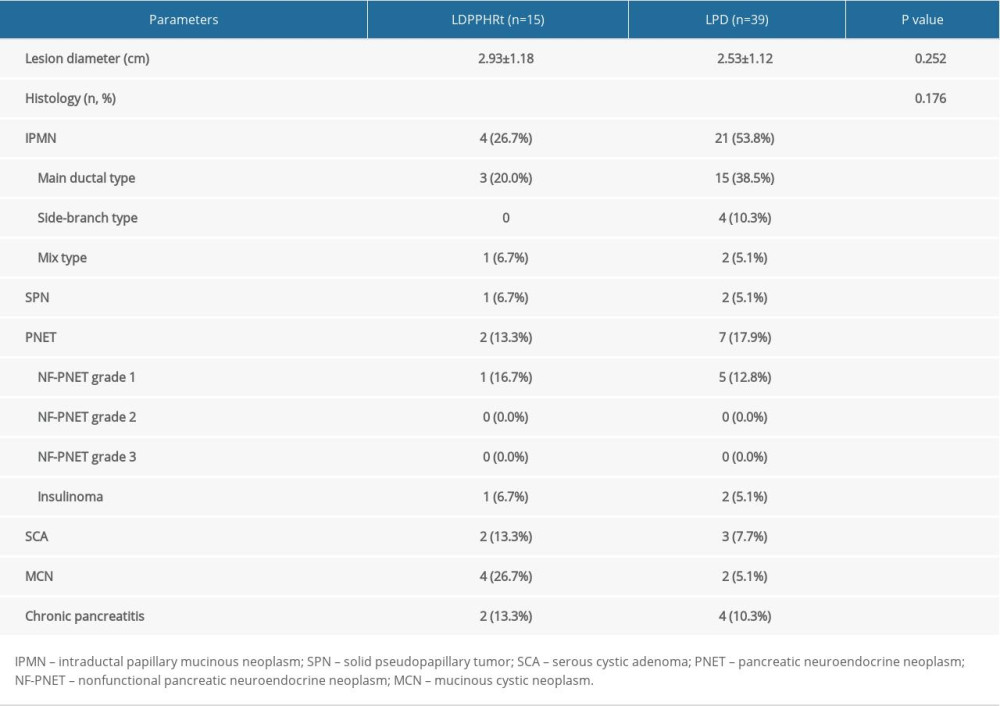
The lesion diameter did not differ significantly between the 2 groups (2.93±1.18 vs. 2.53±1.12 cm; P=0.252). The lesion resection margins were all histopathologically negative. The distribution of pathological diagnosis was also comparable between the 2 groups. In the LDPPHRt group, the postoperative pathology revealed IPMN in 4 patients (26.7%), SPN in 1 patient (6.7%), PNET in 2 patients (1 case of nonfunctional PNET grade 1 and 1 case of insulinoma) (13.3%), SCA in 2 patients (13.3%), MCN in 4 patients (26.7%), and chronic pancreatitis in 2 patients (13.3%). In the LPD group, 21 patients (53.8%) were diagnosed with IPMN, among which 15 cases (38.5%) were of the main ductal type and 4 cases (10.3%) were of the side-branch type. Other diagnoses included 2 cases (5.1%) of SPN, 7 cases (17.9%) of PNET (5 cases of nonfunctional PNET grade 1 and 2 cases of insulinoma), 3 cases (7.7%) of SCA, 2 cases (5.1%) of MCN, and 4 cases (10.3%) of chronic pancreatitis (Table 3).
Discussion
To the best of our knowledge, there have been no studies to date comparing the short-term results of LDPPHRt and LPD. In the present study, we analyzed the short-term outcomes of LDPPHRt and LPD for benign or low-grade malignant lesions of the pancreatic head. We found no differences between the 2 groups in terms of estimated intraoperative transfusion, postoperative stay, postoperative complications, 30-day readmission rates, or 90-day mortality rates. However, LDPPHRt required a shorter operative time compared with LPD. This reduced operative time was due to the fact that, in LDPPHRt, only pancreatic-head resection was conducted, without bilioenteric or gastrointestinal anastomosis.
In the present study, LDPPHRt was found to be predominantly performed on female patients (73.3%) with no previous history of abdominal surgery. This differed from the LPD group, and the difference reflected a selection bias in the patients receiving LDPPHRt. LDPPHRt has the advantage of preserving gastrointestinal integrity, thereby avoiding the need for resection of the duodenum and reconstruction of bilioenteric and gastrointestinal anastomosis. It also has the advantages of common laparoscopic procedures, which require smaller incisions. These are often desired by younger female patients and are associated with a reduced risk of surgical site infection. In the present study, the mean age of LDPPHRt patients was 54.7±13.9 years, which was lower than that of the LPD patients (61.5±11.9 years), although the difference was not statistically significant. The difference in the abdominal surgery history was a reflection of our cautiousness in performing LDPPHRt. To the best of our knowledge, the application of LDPPHRt should be more scrupulous, as LDPPHRt is considerably more technically challenging than LPD when resecting the pancreatic head and preserving the anterior and posterior pancreaticoduodenal arterial arcades and intrapancreatic CBD. The other reason is that the surgeon lacks a direct hold of the pancreatic-head region when encountering intraoperative bleeding in the laparoscopic procedure. Patient selection and extensive experience with LPD were the 2 prerequisites for LDPPHRt. Based on our experience with selecting patients, it is recommended that the lesions should not be located too close to the intrapancreatic CBD and the inferior pancreatic arcades. Special considerations are required in patients with severe pancreatic fibrosis. Our chief surgeon has performed over 200 LPD procedures, and was practiced in uncinate resection, alimentary reconstruction, and management of intraoperative emergencies. LDPPHRt is not without risk in inexperienced hands. As surgeons gain more experience in performing LDPPHRt, it may also be performed in patients who have previously undergone abdominal surgery.
The key surgical advantage of DPPHRt without segmental duodenum resection lies in the protection of the ASPDA and PSPDA and the dissection of the intrapancreatic CBD [9,10]. The preservation of arterial arcades has been well established [11]. In LDPPHRt, strategies for arterial arcade protection have also been extensively described [5]. However, for CBD dissection, studies have shown that bile duct injuries are observed in both open and laparoscopic DPPHRt. In a study by Wang et al., bile leakage was the top postoperative complication, with a morbidity rate of 9% [12]. Schlosser et al. reported the long-term outcome of 76 patients who received DPPHRt without biliary anastomosis, and found that 5 patients (6.6%) developed cholestasis and jaundice [13]. Beger et al. reviewed postoperative morbidity following DPPHR, including duodenal segment resection (DPPHR-S) and DPPHRt, and found that DPPHRt had a higher biliary complication rate (8.4%
The CBD is usually difficult to locate intraoperatively and may be accidentally damaged. In addition, total removal of the nourishing blood vessels and heat injuries may lead to bile leakage and stenosis. In the present study, no bile leakage occurred in the LDPPHRt group. Our strategy to prevent injury of the CBD in the absence of intraoperative application of indocyanine green fluorescence cholangiography was to identify the CBD from the angle formed by the PV and GDA, which we referred to as the inferior CBD triangle. Based on our experience, the inferior CBD triangle was easy to identify once the pancreatic neck was transected and the pancreatic head was rotated 90° to the right. Blidaru et al. analyzed the anatomical peculiarities of the CBD in 150 adult cadavers and 22 human fetuses. They found that the retro-duodenal segment of the CBD has important vascular relations: The PV runs posterior to the CBD; the CHA is on the left side of the CBD; and the GDA descends anterior to the PV and to the left of the CBD. At this level, the ASPDA originates from the GDA, and then crosses the anterior side of the CBD [15]. Thus, anatomically, when lifting the pancreatic head to the right, the GDA would travel to the right side of the CBD, while the CBD itself will appear on the right side of the PV. Then, surrounded by the upper side of the pancreas, the dorsal part of the retro-duodenal segment of the CBD would be situated in the middle of the triangle (Figure 1B). Thus, we named it the inferior CBD triangle to distinguish it from Calot’s triangle [16]. Intraoperative identification of the inferior CBD triangle facilitates intrapancreatic CBD dissection. The dissection could be started at the upper left side of the CBD and continued down to the ampulla by electric hook or scissors. We used electric hook or scissors because dissection using these instruments may be more precise than using an ultrasonic scalpel. Additionally, the electric hook could be used to drag the tissues away from the CBD walls to prevent heat injury. The other benefit of identifying the inferior CBD triangle is that it helps to identify the superior pancreaticoduodenal arterial arcade. The ASPDA travels along the right edge of the triangle and may easily be found. The PSPDA passes right posterior to the CBD and opens at the GDA or the CHA. Dissection of the posterior CBD wall should be performed carefully to protect the PSPDA.
Other techniques to prevent bile leakage include the preservation of a thin sheet of pancreatic tissue around the intrapancreatic CBD to preserve the blood supply of the CBD [12]. Once the CBD is injured during surgery, T-tube drainage, DPPHRt with duodenal and CBD segment resection, or PD could be performed under laparoscopy [12,14].
In the present study, LDPPHRt was performed on patients with benign or low-grade malignant pancreatic-head lesions, including IPMN, SCA, MCN, SPN, and PNET. A study by Cao et al. also reported that LDPPHRt may be suitable for these conditions [5]. DPPHR was initially indicated for chronic pancreatitis [17], after which time an increasing number of studies have been performed to evaluate its performance in pancreatic inflammatory, benign, or low-grade malignant tumors. A series of studies demonstrated that DPPHRt was effective for the treatment of pancreatic cystic lesions [10,18]. The 3 most common types of tumors that have been treated with DPPHRt are IPMN, SCA, and MCN, with IPMN accounting for >60% of total cases [19]. Patients with IPMN, SCA, MCN, SPN, and endocrine lesions are potential candidates for DPPHRt [10]. Total pancreatic-head resection could completely remove the lesion and prevent the development of pancreatic cancer in the remaining pancreatic head. Compared with DPPHRp, DPPHRt may serve as a cancer-preventive strategy by avoiding any possible incomplete extirpation of the pancreatic-head lesions [10]. The majority of the patients with pancreatic cystic or endocrine lesions are younger-aged women with a long life expectancy who prefer smaller abdominal incisions. Thus, LDPPHRt may be more suitable for these groups of patients.
There were certain limitations to the present study. First, this study was retrospective, involving a small number of cases diagnosed with benign and low-grade malignant pancreatic-head lesions. A larger cohort is required to validate the results and conclusions based on long-term outcomes. Additionally, the efficiency in reducing long-term complications, such as CBD stenosis, cholestasis, and jaundice, should be evaluated in future studies.
Conclusions
LDPPHRt was shown to be a time-saving procedure with comparable short-term outcomes to LPD when used for the management of benign or low-grade malignancies of the pancreatic head. Herein, we also reported a new surgical strategy by identifying the inferior CBD triangle when performing LDPPHRt. The inferior CBD triangle is easily identified, and may prove useful in assisting the initiation of the intrapancreatic CBD dissection.
Figures
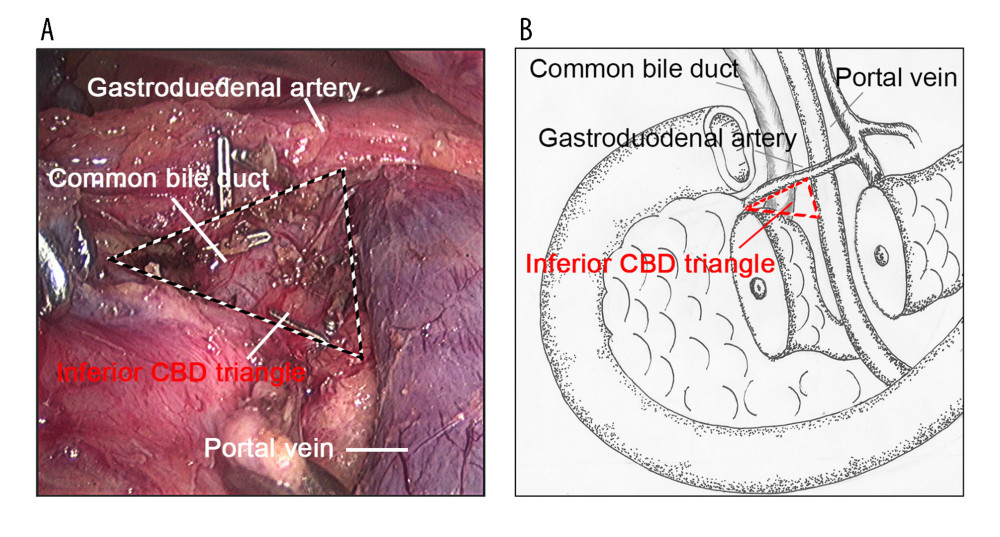 Figure 1. The inferior CBD triangle. (A) Intraoperative images of the inferior CBD triangle. The inferior CBD triangle is formed by the GDA, the portal vein, and the superior edge of the pancreas. (B) Pattern diagrams of the inferior CBD triangle. CBD – common bile duct; GDA – gastroduodenal artery.
Figure 1. The inferior CBD triangle. (A) Intraoperative images of the inferior CBD triangle. The inferior CBD triangle is formed by the GDA, the portal vein, and the superior edge of the pancreas. (B) Pattern diagrams of the inferior CBD triangle. CBD – common bile duct; GDA – gastroduodenal artery. 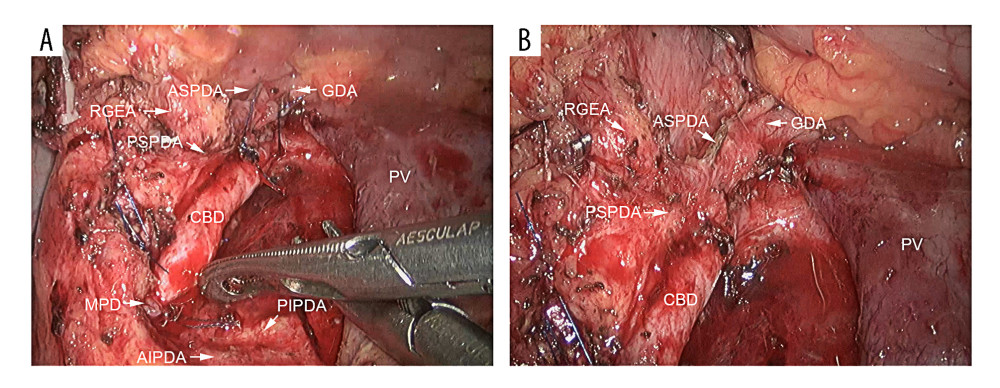 Figure 2. Intraoperative photographs after the pancreatic head was removed using the LDPPHRt procedure. (A) Images showing the superior and inferior artery arcades and the common bile duct after pancreatic-head resection. (B) The ASPDA was ligated and cut during the procedure, while the PSPDA was preserved. ASPDA – anterior superior pancreaticoduodenal arteries; PSPDA – posterior superior pancreaticoduodenal arteries; RGEA – right gastroepiploic artery; PV – portal vein; MPD – main pancreatic duct; AIPDA – anterior inferior pancreaticoduodenal arteries; PIPDA – posterior inferior pancreaticoduodenal arteries.
Figure 2. Intraoperative photographs after the pancreatic head was removed using the LDPPHRt procedure. (A) Images showing the superior and inferior artery arcades and the common bile duct after pancreatic-head resection. (B) The ASPDA was ligated and cut during the procedure, while the PSPDA was preserved. ASPDA – anterior superior pancreaticoduodenal arteries; PSPDA – posterior superior pancreaticoduodenal arteries; RGEA – right gastroepiploic artery; PV – portal vein; MPD – main pancreatic duct; AIPDA – anterior inferior pancreaticoduodenal arteries; PIPDA – posterior inferior pancreaticoduodenal arteries. References
1. Beger HG, Büchler M, Bittner RR, Duodenum-preserving resection of the head of the pancreas in severe chronic pancreatitis. Early and late results: Ann Surg, 1989; 209(3); 273-78
2. Diener MK, Rahbari NN, Fischer L, Duodenum-preserving pancreatic head resection versus pancreatoduodenectomy for surgical treatment of chronic pancreatitis: A systematic review and meta-analysis: Ann Surg, 2008; 247(6); 950-61
3. Nakao A, Harada A, Nonami T, Prognosis of cancer of the duodenal papilla of Vater in relation to clinicopathological tumor extension: Hepatogastroenterology, 1994; 41(1); 73-78
4. Beger HG, Schlosser W, Siech M, Poch B, The surgical management of chronic pancreatitis: Duodenum-preserving pancreatectomy: Adv Surg, 1999; 32; 87-104
5. Cao J, Li GL, Wei JX, Laparoscopic duodenum-preserving total pancreatic head resection: A novel surgical approach for benign or low-grade malignant tumors: Surg Endosc, 2019; 33(2); 633-38
6. Bassi C, Marchegiani G, Dervenis CInternational Study Group on Pancreatic Surgery (ISGPS), The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 Years After: Surgery, 2017; 161(3); 584-91
7. Wente MN, Bassi C, Dervenis C, Delayed gastric emptying (DGE) after pancreatic surgery: A suggested definition by the International Study Group of Pancreatic Surgery (ISGPS): Surgery, 2007; 142(5); 761-68
8. Tan Y, Tang T, Zhang Y: Updates Surg, 2020 [Online ahead of print]
9. Beger HG, Poch B, Vasilescu C, Benign cystic neoplasm and endocrine tumours of the pancreas – when and how to operate – an overview: Int J Surg, 2014; 12(6); 606-14
10. Beger HG, Rau BM, Gansauge F, Poch B, Duodenum-preserving subtotal and total pancreatic head resections for inflammatory and cystic neoplastic lesions of the pancreas: J Gastrointest Surg, 2008; 12(6); 1127-32
11. Miyakawa S, Horiguchi A, Mizuno K, Preservation of arterial arcades during duodenum-preserving total pancreatic head resection for intraductal papillary tumor: Hepatogastroenterology, 2003; 50(52); 993-97
12. Wang C, Liu T, Wu H, Duodenum-preserving total pancreatic head resection without segment resection of the duodenum for chronic pancreatitis: Langenbecks Arch Surg, 2009; 394(3); 563-68
13. Schlosser W, Poch B, Beger HG, Duodenum-preserving pancreatic head resection leads to relief of common bile duct stenosis: Am J Surg, 2002; 183(1); 37-41
14. Beger HG, Mayer B, Rau BM, Parenchyma-sparing, limited pancreatic head resection for benign tumors and low-risk periampullary cancer – a systematic review: J Gastrointest Surg, 2016; 20(1); 206-17
15. Blidaru D, Blidaru M, Pop C, The common bile duct: Size, course, relations: Rom J Morphol Embryol, 2010; 51(1); 141-44
16. Abdalla S, Pierre S, Ellis H, Calot’s triangle: Clin Anat, 2013; 26(4); 493-501
17. Beger HG, Büchler M, Duodenum-preserving resection of the head of the pancreas in chronic pancreatitis with inflammatory mass in the head: World J Surg, 1990; 14(1); 83-87
18. Beger HG, Gansauge F, Siech M, Duodenum-preserving total pancreatic head resection for cystic neoplastic lesions in the head of the pancreas: J Hepatobiliary Pancreat Surg, 2008; 15(2); 149-56
19. Beger HG, Nakao A, Mayer B, Poch B, Duodenum-preserving total and partial pancreatic head resection for benign tumors – systematic review and meta-analysis: Pancreatology, 2015; 15(2); 167-78
Figures
 Figure 1. The inferior CBD triangle. (A) Intraoperative images of the inferior CBD triangle. The inferior CBD triangle is formed by the GDA, the portal vein, and the superior edge of the pancreas. (B) Pattern diagrams of the inferior CBD triangle. CBD – common bile duct; GDA – gastroduodenal artery.
Figure 1. The inferior CBD triangle. (A) Intraoperative images of the inferior CBD triangle. The inferior CBD triangle is formed by the GDA, the portal vein, and the superior edge of the pancreas. (B) Pattern diagrams of the inferior CBD triangle. CBD – common bile duct; GDA – gastroduodenal artery. Figure 2. Intraoperative photographs after the pancreatic head was removed using the LDPPHRt procedure. (A) Images showing the superior and inferior artery arcades and the common bile duct after pancreatic-head resection. (B) The ASPDA was ligated and cut during the procedure, while the PSPDA was preserved. ASPDA – anterior superior pancreaticoduodenal arteries; PSPDA – posterior superior pancreaticoduodenal arteries; RGEA – right gastroepiploic artery; PV – portal vein; MPD – main pancreatic duct; AIPDA – anterior inferior pancreaticoduodenal arteries; PIPDA – posterior inferior pancreaticoduodenal arteries.
Figure 2. Intraoperative photographs after the pancreatic head was removed using the LDPPHRt procedure. (A) Images showing the superior and inferior artery arcades and the common bile duct after pancreatic-head resection. (B) The ASPDA was ligated and cut during the procedure, while the PSPDA was preserved. ASPDA – anterior superior pancreaticoduodenal arteries; PSPDA – posterior superior pancreaticoduodenal arteries; RGEA – right gastroepiploic artery; PV – portal vein; MPD – main pancreatic duct; AIPDA – anterior inferior pancreaticoduodenal arteries; PIPDA – posterior inferior pancreaticoduodenal arteries. In Press
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
08 Mar 2024 : Clinical Research
Evaluation of Foot Structure in Preschool Children Based on Body MassMed Sci Monit In Press; DOI: 10.12659/MSM.943765
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952